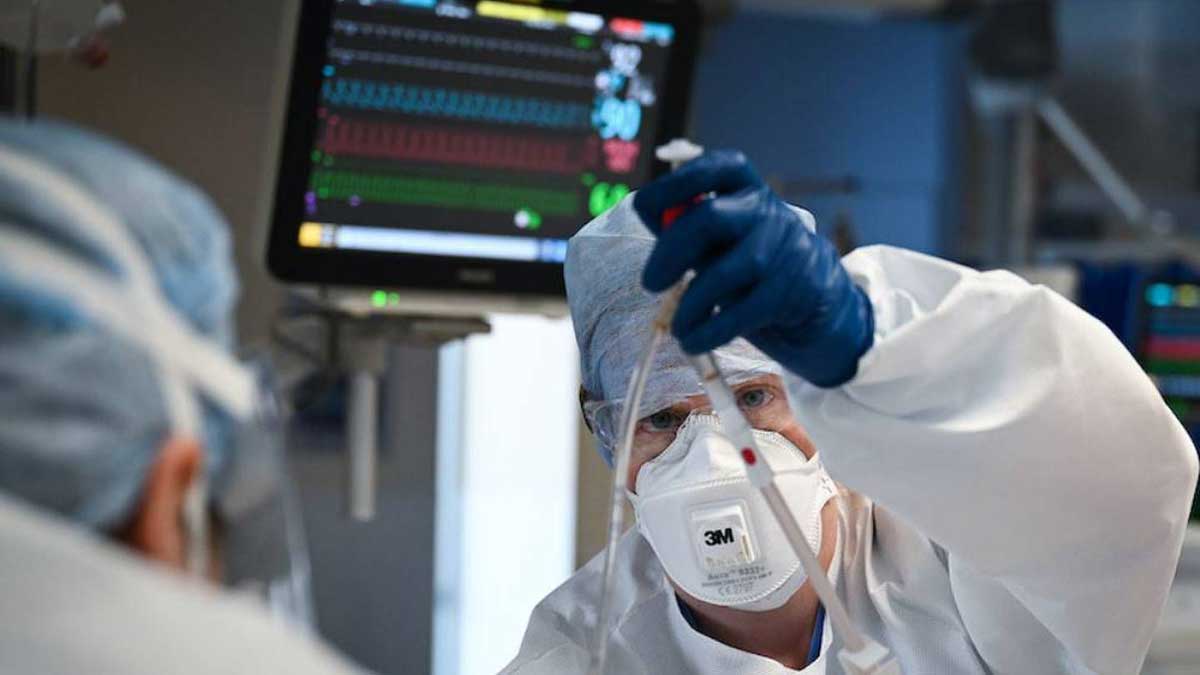
According to recent research, blood types may play a role in whether or not people develop severe symptoms of COVID-19. For example, If your blood group is A, you are more likely to contract coronavirus infections.
The study, which was published in the journal PLOS Genetics, examined at over 3000 proteins to see which ones are causally connected to severe COVID-19. They also discovered six proteins that may lead to severe COVID-19 infections and eight proteins that may defend against severe COVID-19 infections.
According to the study, blood types are determined by one of the proteins (ABO) that was found as having a causal connection to the chance of getting severe COVID-19, implying that blood groups play an important role in whether people develop extreme forms of the disease.
Read more: Fatigue, shortness of breath persist in Covid patients for a year: study
“We investigated a vast number of blood proteins using a purely genetic method and found that a few have causal linkages to the development of severe COVID-19,” stated study co-first author Alish Palmos of King’s College London. “Finding this set of proteins is a critical first step in identifying potentially useful targets for the development of new treatments.”
What did the study reveal?
An enzyme (ABO) that specifies blood group was found to be causally linked to an increased likelihood of hospitalization and the need for respiratory support in the study.
The findings back with prior study linking blood group to a higher risk of mortality, according to the researchers.
Furthermore, together with earlier research demonstrating that the proportion of COVID-19 positive persons who have blood type A is higher, implies that blood group A is a potential for further research, they said.
“The enzyme helps determine an individual’s blood group, and our study has connected it to both likelihood of hospitalization and the requirement for respiratory support or mortality,” said King’s College London study coauthor Christopher Hubel.