We frequently think of physical therapy as a treatment for injuries, post-surgery, the elderly, or chronic pain. Physical therapists, depending on their specialty, can treat a wide range of medical conditions that go beyond the most common reasons for physical therapy treatment. Physical therapy can help restore or improve mobility and movement, control of movement, and reduce the need for prescription medication and surgery for many chronic medical conditions. There are numerous advantages to using physical therapy to treat chronic conditions such as low back pain and osteoarthritis, as well as post-fracture healing.
Physical Therapy in Low Back Pain:
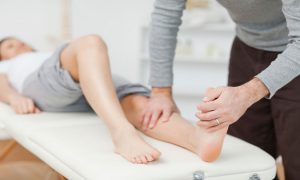
Physical therapy is frequently recommended as a first-line treatment for most types of lower back pain. Physical therapy for low back pain consists of guided therapeutic exercises that strengthen and condition the lower back muscles as well as the spinal tissues and joints.
Physical therapy for back pain typically includes the following short- and long-term goals:
Decrease painful symptoms in the lower back and/or leg
Improve low back function to allow you to participate in daily activities as independently as possible.
Increase the spine’s flexibility and range of motion.
Create a maintenance plan to keep back problems from recurring.
The exercises are designed to provide flexibility and strength training to the entire kinetic chain—the groups of body segments, joints, and muscles that collaborate to perform bodily functions.
Physical therapy helps patients regain their ability to perform daily tasks with little to no discomfort. Physical therapy has been shown in large-scale studies to provide up to 60% improvement in lower back pain and other symptoms.
There are four types of therapeutic exercises for back pain.
Therapeutic exercises are usually performed or learned under the supervision of a physical therapist, and they employ a combination of the approaches described below.
1. Exercises to strengthen the core
The core of the body is defined as the area surrounded by the stomach muscles in front, the spinal and buttock muscles in back, the bottom of the lungs or diaphragm on top, and the pelvic and hip muscles at the bottom. 2 A weak core unevenly distributes weight throughout the spine and into the legs, causing or exacerbating back pain. Core-strengthening exercises help build core muscle strength and endurance, reducing pain and improving lower back functionality.
The pelvic tilt, cat-cow pose, bird dog, high and low planks, crunches, and exercises performed with a Swiss ball are all simple core-strengthening exercises to relieve back pain (or exercise ball).
Read More: Yoga vs Pilates: how to know which one is right for you? – About Pakistan
2. Exercises for lumbar stabilisation
To support the lower body and walk, bend, and twist effortlessly, a strong spine requires strong hips and legs. Muscle inefficiency in the hips and legs has been linked to spinal instability and pain. Stretching exercises can activate and strengthen these muscles, such as the iliopsoas and hamstrings; improve hip-spine coordination; and aid in the transfer of forces across the lower back, pelvis, and legs.
Hamstring stretches, squats, downward dog, planks with leg lifts, and lunges are common hip and leg exercises for beginners with lower back pain.
3. Aerobic workouts
Aerobic or cardiovascular exercise not only keeps your heart healthy, but it also heals your spinal muscles. Cardiovascular exercise entails synchronised movement throughout the body that raises the heart rate, improving circulation, oxygen content within cells, and energy production in tissues. The painful spinal muscles respond by becoming less stiff and more mobile as a result of these mechanisms.
Brisk walking, a stationary bike, and an elliptical trainer are all simple aerobic exercises for back pain. Aquatic exercise can provide low-impact aerobic conditioning. Water’s buoyancy supports the body’s weight, reducing spinal stress and allowing for a greater range of motion.
4. Postural conditioning
Supported posture reduces strain on the body by keeping the muscles and bones in balance. Unsupported posture can be caused by a bad habit, painful symptoms, or poor ergonomics at work or at home. In the spine, incorrect posture can limit the movement of the tendons and muscles, making daily activities difficult and painful. Stretching and strengthening the back and abdominal muscles, as well as the kinetic chain, which help stabilise the spine, are the goals of posture correction exercises.
Calf stretching, seated squats, pelvic tilts, and abdominal strengthening exercises are all common posture correction exercises.
Education, training, strength, flexibility, and endurance are all components of physical therapy. A physical therapist is essential in developing a programme that is tailored to the patient’s needs and limitations. The goal of a therapist is to teach the proper exercise technique so that the patient can perform the exercise on their own.
Back Pain Conditions That May Benefit from Physical Therapy
Unless considered a medical emergency, most lower back conditions may benefit from some form of physical therapy and exercise. The underlying cause of back pain dictates the physical therapy program’s foundation and the types of exercises that must be included.
Axial Back Pain
Axial or nonspecific back pain refers to back pain that does not have a specific cause. This condition is usually caused by a combination of factors, such as poor posture and/or being overweight.
Physical therapy is typically recommended for chronic axial back pain that has lasted more than three months 9 and focuses on stretching and strengthening the lower back while also attempting to eliminate lifestyle factors that may be contributing to the pain.
Sciatica
Sciatica is a collection of symptoms caused by an underlying condition that may irritate or compress a spinal nerve in the lower back, resulting in lower back pain and/or leg pain.
Extension and flexion (forward and backward bending) exercises, lumbar strengthening exercises, and nerve and joint mobilisation methods are common forms of physical therapy and exercise for sciatica.
Pain and healing after surgery
Physical therapy and exercise can help patients recover from spine surgery, return to normal daily activities, and avoid re-injury. Participating in a consistent, guided exercise programme can help the body heal from the surgical procedure and reduce future episodes of back pain.
To begin the post-surgical exercise programme, physical therapists typically recommend abdominal, back, and leg strengthening exercises, as well as some aerobic exercise.
When back pain is caused by a serious medical condition, such as cauda equina syndrome, infection, or spinal tumours, immediate medical or surgical intervention is required.
Duration of a Low Back Pain Physical Therapy Program
The duration of an exercise programme is determined by the severity and duration of the low back symptoms.
Physical therapy for chronic low back pain typically begins with an 8-week programme performed under the supervision of a physical therapist.
Following the guided phase, a longer-term maintenance or rehabilitation therapy that can be done at home is prescribed.
The duration of the guided programme may vary depending on the outcome of the treatment.
To improve the overall pain outcome, physical therapy can be combined with other nonsurgical treatments for the lower back. When combined with a physical therapy regimen, hands-on alternative treatments such as massage therapy, manual therapy, and acupuncture may be beneficial. For some types of back pain, a patient’s doctor may recommend a combination of physical therapy and lumbar epidural steroid injections. Pain relievers may also be prescribed by doctors. Physical therapists may recommend self-care measures such as heat and cold therapy to reduce pain and inflammation and promote tissue healing.
Read More: The use of manual therapy techniques to improve range of motion and decrease pain – About Pakistan
Physical Therapy in Arthritis:
Physical therapy (PT) is a promising arthritis treatment option.
Working with a physical therapist can help you manage your symptoms, improve your mobility, and enhance your physical function. They will also teach you specific exercises and techniques to help you move with less pain and ease.
How can physical therapy help with arthritis treatment?
PT for arthritis relieves symptoms and improves movement quality. This makes performing everyday movements easier.
PT is typically included as part of an arthritis treatment plan that also includes:
Medication
Supplements
Topical treatments
Your posture, muscle imbalances, and body mechanics will also be evaluated by a physical therapist. They will teach you how to move better in order to avoid injury, reduce pain, and align your body.
A physical therapist can design a stretching and exercise programme that will help you:
alleviate discomfort
broaden your range of motion
enhance movement patterns
It will include exercises to strengthen the muscles surrounding the joints, which can improve function and reduce joint stress.
Physical therapy for arthritis may also be beneficial:
make a home workout routine
improve your overall fitness level, increase endurance, reduce stiffness, and fatigue, improve balance and stability, and increase coordination
Best types of physical therapy for Arthritis
The best type of physical therapy for you will be determined by your concerns and treatment objectives. Look for a physical therapist who specialises in arthritis or a particular body part, such as the hands or feet.
A physical therapist may instruct you on how to use:
weight machines, aerobic exercise machines, and other pieces of equipment such as foam rollers, exercise balls, and resistance bands
They may also recommend and teach you how to use an assistive device. Massage, joint mobilisation, and electrotherapy are examples of passive PT treatments that promote relaxation.
Can physical therapy aggravate arthritis?
Physical therapy seeks to improve function while alleviating arthritis symptoms. Treatment should not aggravate your symptoms or cause pain.
However, you may find some of the exercises difficult, especially at first. A moderate amount of muscular discomfort or soreness is normal after or during a PT session.
Discuss your treatment response and pain tolerance with your physical therapist. Inform them if you experience worsening symptoms, severe pain, or difficulties during or after a session.
Your physical therapist can make the necessary changes to your treatment plan. They may employ alternative techniques or reduce the frequency and intensity of your sessions.
Exercise safety tips for people with arthritis
Exercising has numerous benefits for arthritis, as long as it is done safely. Consult your doctor or physical therapist before beginning an exercise programme for arthritis. They can suggest appropriate exercises and modifications.
Make an effort to stretch. Warm up before each session and cool down afterwards. Stretch all major muscle groups before working out, paying special attention to joints prone to pain and stiffness.
Take your time. Begin with short workouts, work your way up gradually, and stay within your limits. Pay attention to your body, especially if you’re experiencing a flare-up, and take as many breaks as you need. Take plenty of rest days in between workouts.
Perform low-impact exercises. These activities relieve joint stress or pressure. Swimming, aquatic therapy, and gardening are among them. Exercises to improve strength, balance, and flexibility can also be included. Exercises that cause severe pain or worsen your symptoms, such as swelling, pain, or stiffness, should be avoided.
Read More: Physiotherapist vs Chiropractor: How Do They Differ? – About Pakistan
Conclusion:
Physical therapy provides the same benefits to people suffering from any chronic disease. To reduce the risk of falls and improve mobility, a physical therapist will work with each individual to improve strength, walking ability, and balance. Physical therapy can also help patients increase their physical activity to a level that is comfortable for them. Physical therapy for someone suffering from OA focuses on improving movement, balance, and coordination.